Viruses and virally derived particles have the intrinsic capacity to deliver molecules to cells, but the difficulty of readily altering cell-type selectivity has hindered their use for therapeutic delivery. Here, we show that cell surface marker recognition by antibody fragments displayed on membrane-derived particles encapsulating CRISPR–Cas9 protein and guide RNA can deliver genome editing tools to specific cells. Compared to conventional vectors like adeno-associated virus that rely on evolved capsid tropisms to deliver virally encoded cargo, these Cas9-packaging enveloped delivery vehicles (Cas9-EDVs) leverage predictable antibody–antigen interactions to transiently deliver genome editing machinery selectively to cells of interest. Antibody-targeted Cas9-EDVs preferentially confer genome editing in cognate target cells over bystander cells in mixed populations, both ex vivo and in vivo. By using multiplexed targeting molecules to direct delivery to human T cells, Cas9-EDVs enable the generation of genome-edited chimeric antigen receptor T cells in humanized mice, establishing a programmable delivery modality with the potential for widespread therapeutic utility. Cell-specific molecular delivery with enveloped delivery vehicles enables genome editing ex vivo and in vivo.
Research and publish the best content.
Get Started for FREE
Sign up with Facebook Sign up with X
I don't have a Facebook or a X account
Already have an account: Login
 Your new post is loading... Your new post is loading...
 Your new post is loading... Your new post is loading...
|
|





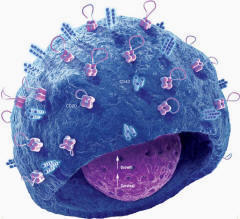














A new precision-targeted delivery method for CRISPR-Cas9, published in the journal Nature Biotechnology, enables the genetic editing of highly specific subsets of cells while still inside the body: a step towards a programmable delivery method that would eliminate the need to erase patients' bone marrow and immune systems before giving them modified blood cells. The delivery method, developed at the University of California, Berkeley, laboratory of Jennifer Doudna, co-inventor of CRISPR-Cas9 genome editing, involves wrapping Cas9 editing proteins and guide RNAs in a membrane bubble decorated with pieces of monoclonal antibodies that target specific types of blood cells. As a demonstration, the researcher targeted a cell of the immune system, a T lymphocyte, which is the starting point for a revolutionary cancer treatment called CAR- T cell therapy. The research team treated live mice equipped with a humanized immune system and transformed their human T cells into CAR T cells capable of targeting and eliminating another class of immune cells, the B cells.